Corneal recovery is a key property of ocular irritation classification schemes used in the regulatory arena. However, no current validated non-animal ocular irritation test methods or prediction tools are able to predict corneal recovery in a manner consistent with the animal tests historically employed. Whereas some efforts have been made to demonstrate recovery with in vitro or ex vivo corneal models, the current state of these technologies do not support demonstration of recovery of the corneal stromal elements, which are key to discriminate between moderate and severe irritants.
Fortunately, the Depth of Injury model of Jamie Jester and James Maurer provides the basis for recovery/non-recovery predictions without the need to maintain ex vivo tissues for extended periods. Depth of Injury analyses can readily be performed on corneal histology sections obtained from the Bovine Corneal Opacity and Permeability assay (BCOP), and IIVS’s scientists have over 20 years expertise in the use of histopathology to supplement the BCOP assay.
Several of the regulatory schemes for grading eye irritation potential in vivo use time-to-recovery as a primary driver of classification. However, current validated in vitro ocular irritation test methods are designed to classify test materials based on measurements of direct ocular damage, and they do not directly assess corneal recovery. For some test materials where the initial injury is does not result in severe damage, the inability of the cornea to fully recover from such injuries would be the basis for assigning a severe/corrosive eye irritation classification. There are however potential approaches to assessing the potential for corneal recovery. Some efforts have been made to measure recovery with in vitro or ex vivo corneal models, by focusing on the reestablishment of a corneal epithelium, but corneal recovery in vivo involves much more than re-epithelialization, especially when assessing ocular damage from moderate and severe irritants. The current ex vivo models suffer from progressive stromal swelling and degradation of the stromal elements – exactly those tissues required to discriminate among moderate and severe irritants. Additionally, these models do not address the inflammatory process that occurs in vivo, or its significant impact upon corneal recovery downstream. Accordingly, these limited approaches do not present a mechanistically-relevant model for resolving among moderate and severe irritants.
Fortunately, the initial depth of injury model of Jamie Jester and James Maurer provides the basis for recovery/non-recovery predictions without the need to maintain ex vivo tissues for extended periods.
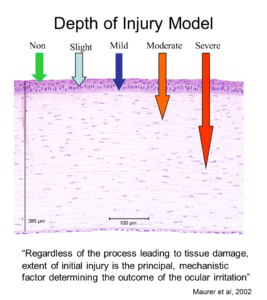
Depth of Injury Model
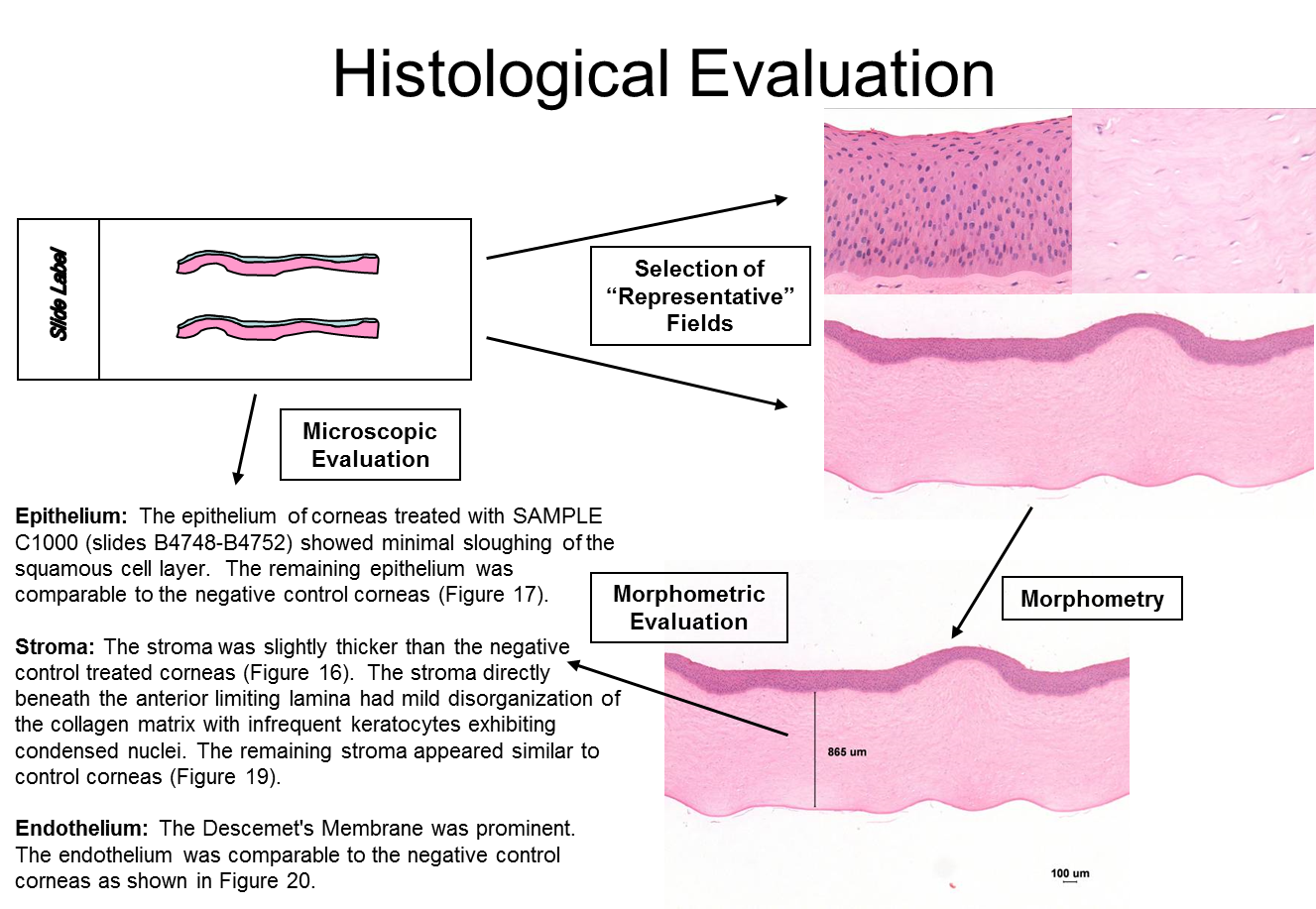
Depth of Injury analyses are performed on corneal sections from the Bovine Corneal Opacity and Permeability assay (BCOP). Jester and Maurer have shown for a range of chemical classes that depth of injury in the early hours after exposure can be predictive of the eventual degree and duration of the ocular lesions. Epithelial damage alone, in the rabbit cornea, is associated with expected recovery provided the basal lamina is intact. Similarly, changes to the surface epithelium (squamous and upper wing cell epithelium) in the BCOP assay are usually not predictive of lasting corneal changes in vivo. Deeper injury into the stroma has more serious consequences, while a full thickness injury including damage or loss of the endothelium would be predictive of a severe injury.
IIVS has lead the use of histopathology to supplement the BCOP assay and routinely provides detailed descriptive pathology reports to present on the nature and degree of observed corneal changes. An integration of the observed corneal changes with the objectively determined corneal opacity and permeability measurements provide the basis for industry toxicologists and formulators to fully appreciate the impacts of their candidate formulations on corneal tissues.